
Do you suffer from period pain? Have been told that it is a normal part of being a woman!
Do you suffer from pelvic pain throughout the month?
Do you have pain with sex? Is this affecting your relationship?
Do you have pain when passing urine or opening your bowels?
You are not alone!
Pelvic pain is a very common problem experienced by thousands of women. It is one of the major complaints in as many as 20% of all presentations to general gynaecology clinics.
PAIN does not discriminate. The pain can be exacerbated by certain activities or during certain periods. Women report pelvic pain with sexual activity, passing urine or opening bowels. Often, multiple pathologies can co-exist and may lead to chronic pelvic pain. These patients require evaluation by a specialist gynaecologist who is an expert at dealing with pelvic pain. Non-Gynaecological pelvic pain may arise from the digestive tract, ligaments and or muscles of the pelvic floor. Rarely, irritation of pelvic nerves can also be the cause of pelvic pain.
Clearly, it is a common and distressing symptom, more so because it can affect a woman’s ability to work, her self-image, her relationships and her sexuality. If ignored, it can develop into chronic pelvic pain. These women get absorbed into the world of pain treatments, causing disability which eventually lead to dependency.
Endometriosis, one of the most important caused of pelvic pain, occurs when tissue that lines the inside of the uterus grow (implants) outside of the uterus, in other organs or structures in the body. Oestrogen is a hormone produced mainly by the ovaries causing growth of the inner lining of the uterus (the endometrium). Endometriosis thrives in an oestrogenic environment. With each menstrual cycle, these implants become inflamed, bleed and cause pain. The disease can lead to scarring and finally resulting in pelvic adhesions that are responsible for infertility. Similarly, endometriosis is detrimental to the ovary leading to decreased and or poor quality of eggs, again contributing to subfertility.
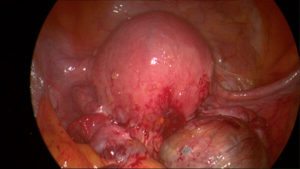
Pelvic Endometriosis is found in about one-third of women undergoing laparoscopy for chronic pelvic pain. Published studies show a diagnostic delay of 8.5 years from onset of symptoms to the eventual diagnosis of endometriosis!
This means that women can suffer for 8.5 years before a diagnosis of endometriosis is made, and appropriate interventions are carried out.
Some of the common reasons for the delayed diagnosis are seen below:
1: Women thought that it was normal to have period pain
Young girls often put on a brave face and bear the pain that has been normalised by society, in fear of appearing weak.
2: Women were told that symptoms were normal.
Often, family members and friends who mean well, will confirm this perception. Multiple treatments with pain medications and oral contraceptive pills are prescribed at the first point of medical contact. The notion that they are unable to cope with normal, albeit painful, periods causes women to take harmful levels of analgesia.
3: Hormonal drugs provided temporary relief
Yes, these medications do provide temporary relief, but there has often been no diagnosis for their pain. It is akin to giving paracetamol for fever without knowing the cause of the fever.
4: Inadequate diagnostic methods are used
When pelvic pain occurs, almost everyone gets a pelvic ultrasound scan, and most are reported as normal. This reinforces the notion of normality, further delaying the diagnosis of endometriosis. Unless a woman has large endometriomas (endometriotic cyst in the ovary), ultrasound is not sensitive enough to pick up other forms of endometriosis.
Despite our advances in medical science, Laparoscopy and biopsy of the endometriotic implant are the gold standard in diagnosing endometriosis.
Management:
Women with acute episodes of pelvic pain should be assessed quickly. They should present to the Emergency Department to rule out and treat other causes of pelvic pain, e.g. ectopic pregnancy, appendicitis, etc .
Identifying the cause of the pain is the most important step. While women do not like having endometriosis, they are relieved to find a reason for their suffering. Early detection, early diagnosis, and early intervention are the best methods for endometriosis management.
Pelvic pain can control a woman’s life!
Here are a few steps that can help to take control of Pelvic pain secondary to endometriosis:
1 Identify the cause of the pain: – See your Primary health care provider early. If he or she have ruled out other causes of pelvic pains, such as infections; Ask leading questions such as –
“Do you think, I could have pain due to Endometriosis?”
“The Contraceptive pills have not helped with relieving pain, Could this be endometriosis?”
2 Maintain proper weight: Engage in physical activity, stay active, stay working. Body fat is a secondary production site for estrogen, so being overweight often means excess estrogen that then can worsen endometriosis.
3 Diet: While there are no dietary guidelines for prevention or treatment of endometriosis, studies have shown that there is a lower risk of developing endometriosis with a high intake of green vegetables and fruit. Similar studies also showed an increased risk with intake of beef or other red meat or ham. Avoid all soy products. Soy contains phytoestrogens that mimic estrogen in the body and can potentially worsen the endometriosis.
4 See an Endometriosis Expert: If you do experience symptoms suggestive of endometriosis, seek evaluation from an expert in endometriosis who is a part of multidisciplinary team that deals with all aspects of endometriosis. Part of the problem is, where can you find the medical help that you desperately need? Sadly, there is no medical degree that is required to be called an ‘Endometriosis Expert’. The Royal Australian & New Zealand College of Obstetricians & Gynaecologists (RANZCOG) and the Australasian Gynaecological Endoscopy & Surgery Society (AGES) , however, have guidelines which state that a surgeon should be acceditated to Skill Level 6 prior to performing advanced operative laparoscopy for endometriosis. You can download a copy of the full text by clicking here.
An expert in Endometriosis should primarily understand the disease process and its impact on the women’s life. He should also have a combination of excellent surgical skills, thorough knowledge of endometriosis and its current treatments.
Treatment by an endometriosis expert may help you avoid years of misdiagnosis or inadequate treatments!
Follow my posts on Google
Contact us at AEVAFEM for more information
At AEVAFEM, our specialists will take the time required to make you feel comfortable, alleviate the uncertainty of having a gynaecological procedure or surgery and help you make an informed decision on the best treatment solution for you.
Dr Yogesh Nikam is a Specialist Gynaecological & Uro-Gynaecological Surgeon
Dr Warren Chan is a Fertility Specialist & Gynaecological Surgeon
Call 1300 724 380 to make an appointment.
